Irene Overton
My Journey So Far
By Irene Bailey Overton March 2004
 Everyone has a story to tell. This is mine! This bumpy and challenging journey I have gone through actually began in Jan. of ’96 when my Dad passed away somewhat unexpectedly…. It was a sad shock to our close family. My Mom was already showing signs of confusion when Dad passed away, and her doctor told us it was Alzheimer’s Disease. She wouldn’t (and probably shouldn’t) stay alone and she needed more help with most things. My two brothers, Woody and Marvin and myself (my sister, Nancy, lived away so was not able to physically help too much) did everything we could for her, including taking turns staying nights with her and making sure she had meals, taking her on errands, just keeping her company, etc. Even though it was stressful at times being a caregiver, and it put a strain on our own family lives, we wanted to help her so much. We were glad we were able to be there for her and were frustrated that we couldn’t do.
Everyone has a story to tell. This is mine! This bumpy and challenging journey I have gone through actually began in Jan. of ’96 when my Dad passed away somewhat unexpectedly…. It was a sad shock to our close family. My Mom was already showing signs of confusion when Dad passed away, and her doctor told us it was Alzheimer’s Disease. She wouldn’t (and probably shouldn’t) stay alone and she needed more help with most things. My two brothers, Woody and Marvin and myself (my sister, Nancy, lived away so was not able to physically help too much) did everything we could for her, including taking turns staying nights with her and making sure she had meals, taking her on errands, just keeping her company, etc. Even though it was stressful at times being a caregiver, and it put a strain on our own family lives, we wanted to help her so much. We were glad we were able to be there for her and were frustrated that we couldn’t do.
Looking at my background, I had a pretty typical life. I went to a local college for two years. Just before I went off to East Carolina University, I met the love of my life. I went on to ECU and finished school, came home and Randy and I got married when I was 24. I worked for 17 years as the Recreation Therapist/Activities Director in a nursing home in a job I absolutely loved! My health history, on the other hand, has always been a little unusual, ever since I was young. I had some unusual “female problems” that began when I was 6 years old, that resulted in a surgery then and another surgery when I was 18, which prevented me from having children. I had stomach problems, circulation problems in one leg and a lot of sinus and respiratory problems over the years. I knew I had some type of lung problem. When I was 18 and received a chest x-ray at Duke University Medical Center, (while I was being treated for my other problems), it revealed abnormal “mild fibrosis in my lungs”. My lungs posed little or no problem for years but gradually, I could feel my breathing getting more difficult. In early ’99, I was having a lot of health problems, a severe case of flu, skin rashes, bladder infections and stomach problems. I was loosing weight but more evident, my breathing was becoming much worse. On my 40th birthday, in April, I decided I had to attack everything head on. I had been in denial and trying to hide that my breathing was so bad. Others saw it but I didn’t want to admit it. I was spending almost all of my free time taking care of my Mom. I was too busy to be sick!I went to a local pulmonologist and was misdiagnosed. He told me I would be fine, I had some minor problems and I needed more exercise….this was June of ’99.I didn’t have the energy or I would have gotten really upset about a pulmonologist not recognizing my real problem, however I just wanted to feel better and breath again.
 Finally I was referred to an excellent doctor (and group of doctors) in Norfolk , Va. on Aug. 23rd, 1999, about an hour from my home. I went to him armed with all my tests and x-rays from the other doctor. He was shocked at what I had been told by the other doctor and told me on my first visit that he thought I had Idiopathic Pulmonary Fibrosis and Secondary Pulmonary Hypertension and he thought I needed to get listed for a double lung transplant ASAP. He sent me for more tests that same day. A friend had come with me that day to my appointment and needless to say, we were both in a sort of shock on the way home. Thank goodness he directed me to the right track to get a lung transplant evaluation and then listing for lung transplant.
Finally I was referred to an excellent doctor (and group of doctors) in Norfolk , Va. on Aug. 23rd, 1999, about an hour from my home. I went to him armed with all my tests and x-rays from the other doctor. He was shocked at what I had been told by the other doctor and told me on my first visit that he thought I had Idiopathic Pulmonary Fibrosis and Secondary Pulmonary Hypertension and he thought I needed to get listed for a double lung transplant ASAP. He sent me for more tests that same day. A friend had come with me that day to my appointment and needless to say, we were both in a sort of shock on the way home. Thank goodness he directed me to the right track to get a lung transplant evaluation and then listing for lung transplant.
In the meantime, we are still trying to take care of my Mom. She didn’t understand what was going on with me because of her confusion. I was still working full time, as the Activities Director/ Recreation Therapist at a nursing home, and trying to maintain my life as normal as possible, while I had a million thoughts running around my head about what lay ahead. At the end of the day, I was worn completely out by being so busy and struggling to breathe. I really missed my Mom now…. I wanted to talk to her about things and couldn’t really because she didn’t understand what was happening. On Sept. 23rd, 1999, I was admitted to Sentara Norfolk General, in Norfolk , Va. for an Open Lung Biopsy, (for a definite diagnosis) supposedly a simply procedure that tuned into a 27 day stay, including ICU. I developed a Staph infection and also a severe reaction to TPN, (a nutritional supplement I was being given by IV because I couldn’t eat solid food) and this sent me into Respiratory Distress and into ICU. It was determined that I am allergic or cannot tolerate anything with Fat Lipids in it, which TPN has. I also got Pancreatitis on top of all this. I was put on the “big gun” antibiotics to try and clear everything up. This was when I knew my life would never be the same. For the first time, I was on O2 (oxygen) on a continuous basis, although I had actually needed it sooner. I knew I couldn’t go back to work and it was recommended I apply for Disability. I knew that my family (my husband, my brothers and sister and my sister-in-laws and nieces and nephews and my husbands family) and friends and church would be supportive, but I never realized how much. They were absolutely Wonderful! During this hospital stay I was sooooo sick and so scared. I couldn’t sleep, I was anxious, etc. Someone was with me almost all the time, because I was such a mess both physically and emotionally. Our home is about an hour from the hospital, so I was fortunate that I had lots of family and friends visiting. They went ahead and evaluated me for transplant while I was there, but I was so sick that the evaluation process was hardly even an issue to me. Mainly I just remember them taking a heck of a lot of blood (18 tubes one time) and doing a heart catherazation and a few other tests. My sister lives in South Carolina , and at the time her Congressman was Lloyd Spence, who had undergone a double lung transplant several years earlier. She did not know him personally but knew about his personality and gentle nature. She called his office and asked his secretary if maybe he could drop me a note of support and a word about how well he was doing. She said, no, I am sure he will want to call her and talk to her. He did, that same day. He was so encouraging. I could barely talk to him because I was so sick but he talked and I listened. He told me that he got his life back and I could too, but I would have to listen to my doctors and do just what they tell me too. At that time I didn’t realize the importance of his words! I really thought at times that I was going to die while I was in there, I had never been this sick ever…. I remember I prayed out loud with family members about dying, about going on to a better place if that was Gods will. I had so much support from everywhere and so many prayers it was unbelievable and overwhelming.
During the listing process, of course they talk to your insurance company, and mine denied coverage of the transplant at first. My sister had kind of taken the lead in some of the paperwork and financial issues. She, along with some advice from the coordinator and financial person in the Transplant Center , appealed their denial. In just a few days they reversed it and approved it…. Hooray!! I really remember very little of this time frame even though they were keeping me well informed… I was just plain sick! I was officially listed for transplant in mid October of 1999, and came home from the hospital on Oct. 20. I was told to get my strength back, try to stay healthy, and hopefully I would have a new set of lungs in 18 months or so!
The Wait
I was scared, tired, weak and stressed out. I was thinking about my Mom, my husband, my marriage, dealing with insurance (they weren’t too crazy about spending the amount of money they were about to spend on me), dealing with no longer working, being on disability, and hauling O2 around with me for the first time. All the usual things a new person waiting for a transplant goes through. My life was completely different in a very short amount of time. It didn’t even seem real. I kept thinking I would wake up from the dream I was having. I am generally a positive person with a good outlook, always, seeing the glass half full, but so much had changed so fast, this was quite a strain on me. The Transplant Center and my family recommended I go to a therapist to work on stress and coping management. I was worried about the surgery, I was worried about the ventilator, and I was worried about money. Heck, you might as well say I was worried about everything! As worried as I was however, I never once thought I was making the wrong decision about having the transplant. The only choice I had was do I want to live or do I want to die. I wanted to live, and knew that somehow I would learn to handle or cope with the stress of it. The sooner I got “the call” the better. Of course, we were still trying to care for my Mom, bless her heart. I felt so guilty that I was not able to help much. My brothers had to assume all of the responsibility for her care. I missed being with her. I couldn’t go sit with her like I had before, because she was a smoker and she didn’t understand about my oxygen. I was able to see her on a limited basis.
As hard as it was, I did try to stay positive. My transplant (tx) center and doctors were convinced I was a great candidate for transplant and thought I would do well with it. One day I would have my life back. However, they did stress that a transplant is not a magic cure all for my illness, but trading one set of problems for another set that is easier to deal with and manage. They also educated me to facts about survival rates for lung transplant patients, which I didn’t really even pay too much attention to. I prayed and I tried to keep in my mind that things happen for a reason, and good things can come out of bad times in our life. I tried to read positive things to help me stay positive. The poems,“It’s in the Valley’s I Grow” and “Unfolding the Rose” were very inspirational poems someone had given me that helped me a lot. I kept thinking and believing He would get me through this ordeal. I did not understand what was happening to me, but I knew that as long as He did that was what mattered. I knew also to stay healthy I had to stay positive and could not drown myself in self-pity. Slowly I began to feel better and got some strength back. I participated in Physical Therapy for a while because I had gotten so weak in the hospital. My sister was such a blessing and stayed with Randy and I for a little while until I got myself going again. It was quite an adjustment learning to function around the house with the oxygen on at all times and taking an oxygen tank with you everywhere you went. I tried to stay busy and get out as much as possible. My husband was great about trying to help me not stay cooped up. We still went out to eat, out with friends, etc. I could still drive some around our little town, and do a few errands on my own, as long as I didn’t have too far to walk. If we went to bigger stores or malls, I used a wheelchair or motorized cart in most cases. If I were in that motorized cart, you better watch out…nothing was safe!
With me not working, and we had bought a new house a year before, and the huge cost of pre and post tx care and medication, money was a big worry. Randy had also just started a new job just a few months earlier. I remember someone told me “don’t worry about money” and I thought, are you crazy??? It’s a big concern… you have to pay for portions of the hospital care, meds, and bills, travel, and etc, etc, etc. And although I was getting Disability it was not nearly my regular income. The community rallied around me in an astounding way, planning fund raisers, and other forms of assistance. I just could not believe the generosity I was seeing. I was so thankful for them for all they were doing for me. God put some wonderful people in my life!
We had to put my Mom in a rest home not too long after I was discharged from the hospital. It was such a difficult decision, but my family had too much on them with providing care for her and me also. Plus they were having their own issues they were dealing with. (My brother Marvin had a lot of flooding damage from Hurricane Floyd that he was trying to get straight and my sister and other brother were dealing with her own health problems.) I was feeling bad because I could no longer provide any help except emotional support (and I myself was a wreck). Mom hated the rest home and didn’t understand why she was there (oh the stress and guilt). I would go to see her with my O2 tank and she would beg me to take her home and ask me why I had that tube.
I hated imposing on people…. I was used to being the caregiver to my Mom and at my job, now I was the receiver of the care, but with the help of my therapist I slowly learned to be gracious and accept peoples acts of kindness more easily.
For Christmas of 1999, my family got me a computer, which was a great thing for me! I joined Secondwind Lung Transplant Support Group and saw that others were going through the same thing and saw that some others were worse off than I was. Best of all, I saw that there were many people who had already had transplants who were doing great! This was such a positive for me! The computer was good also, because it was company for me, I could research things, play games and occupy my time. I had never before had so much time on my hands.
I had been going to rehab at my transplant center, Norfolk General, 3 times a week, to help maintain my strength for my transplant. However, besides Idiopathic Pulmonary Fibrosis, I also had Secondary Pulmonary Hypertension. This caused pressure in my lungs, and it was increasing, causing stress to my heart. They made me stop rehab and I was told not to exercise any… just take it easy as much as possible… this was Jan of 2000. I hated stopping the rehab. I knew I needed to be in good shape for the transplant, but they said the exercise was becoming detrimental to me. I also hated to stop because I had met other people there who I had become friends with whom were also waiting for a transplant, including my young friend Stephan who was 18.I could see myself getting worse off and weaker, I was having stomach problems, which caused reflux. They were trying to get me to gain so I would be stronger at the time of my transplant, and I was losing. I was drinking Ensure along with high calorie meals, but it was so hard to eat, I had to force myself. They told me at one point that they may consider me for a Heart/Lung Transplant if the pressure in my lungs didn’t improve. They thought I might be doing permanent damage to my heart.
Everyone could see I was getting worse fast and the tx center said this happens sometime because IPF (my disease) is very unpredictable. The waiting list was not moving…. I was later told that at this point some people really thought I would not make it long enough to get the call as I was declining so rapidly. I felt like I was knocking on Heavens door. I was in the hospital a couple of times for various reasons, at one point I really thought I was having a nervous breakdown. And to top it off, my dog, that was like my child, of 15 years, died!! I was still trying to visit my Mom, who was much worse. She had broken her hip on Christmas Eve, she wouldn’t eat… on my visits I would try to feed her. She rarely recognized any of us. I kept on moving slowly, dragging my oxygen tank around with me. My family didn’t like me driving myself places alone, but knew it was important for me to keep some independence. It was very difficult for me to get the oxygen in and out of the car by myself.
My Mama was admitted to the hospital again for a subdural hemotoma with bleeding of the brain from a fall….she was there a few days and went back to the nursing home. Despite all of this I still tried to be positive and up beat, although I was scared to death, tired and stressed out. What else could happen???? On March 1st I was admitted to Norfolk General, with all kinds of symptoms, throwing up, stomach problems, breathing problems, etc…. I stayed there until March 9th. On the 16th the rest home called. Mom was lethargic, and was sent to the hospital again, and given 24 hours to live, but she hung on. My brother Marvin was away on a well-deserved cruise, so we called him and he got back here as quickly as possible. I was going to see her as often as I could, having to go in a wheelchair and someone to help me because I couldn’t walk that far anywhere. On March 23rd I had an appointment at Norfolk with Dr. Burke. My brother Woody took me. My lung pressures were even higher… they told me to REALLY take it easy… Well, easier said than done. Mom died the next day. This was like the second time I had seen her die. Once I witnessed the slow death of the Mom I knew, from the process of Alzheimer’s and again now. I felt awful that I couldn’t help my brothers and sister with arrangements… I just showed up for everything and felt like everything was in a haze. Just getting ready to go somewhere was an ordeal for me and wore me out. Those few days were not good. Yet… I kept thinking…. I am going to get through this. I kept praying for the Lord to get me through. It seems every time I thought it was at all I could do, I found I could do more. I had surrendered everything to Him and told Him I was tired and He would have to sustain me and He did! He helped me through every single storm, one day at a time, with the help of a lot of Guardian Angels I had acquired! At this point, although I was still stressed, tired and weak… I had come to terms that I was failing fast and may not make it to transplant. I just trusted in the Lord to do what was best for me. The therapist I was seeing told me he could see that although I was stressed I was not as scared at this point (there is a difference). I was still not sleeping well at all and had to be in a wheelchair for most places I went. I was able to walk around the house and short distances. My family, husband and friends were so concerned and I hated to see them worrying about me.
During all of this, I was dealing on an almost daily basis with insurance issues, Disability paperwork, etc. I tried to take care of these things myself as much as possible because although stressful it gave me something constructive to do. Taking care of insurance was (and still is) almost a full time job. My sister and sister-in-law were helping me in these areas as well. I would have trouble at times with phone calls, because talking a lot even with the O2 made me very out of breath. My brothers and some of my friends were busy taking me to Norfolk to appointments. Randy was not able to take me on many of the out of town appointments because it was hard for him to get away from his job. He had started a new job with Lance, Inc just a couple of months before I was diagnosed.
During this period, several different groups were doing fundraisers for me. This was so appreciated, but also difficult for me. I didn’t feel like I was worthy of all the attention I was getting and all that people were doing for me…. Ruritans Club, my church, VFW, my Beauty Salon, friends, and even people I didn’t know, etc. They raised over $15,000.00 for my transplant fund that we had set up, to help pay bills, meds, expenses, etc. We sat up a Transplant Trust Fund to hold the monies that were donated. With my trust fund, a family member or myself could not be the trustee of the fund, and my wonderful friend and another of my many Guardian Angels, Sherree, agreed to manage this fund and paid my bills out of it when needed.
My father-in-law was also having health problems. On May 10th, he had a “5 bypass” open-heart surgery and he came home on the 16th of May. That same day Guardian Care, where I use to work, gave me a special award at a banquet, for my work there. This was very emotional. The next day, May 17th I had no energy, and slept almost all day. I think I was physically and emotionally drained. On the 18th I had another bad day. That evening I went out on the porch with my O2 tubing trailing behind me, to try to read some. I ended up coming in and sitting on the couch crying. Randy asked what was wrong. I said to him…” I can’t do this any more, I am tired, I don’t think I can keep this up, I want something to happen one way or the other.”
The Call
The next day, the 19th was our 16th wedding anniversary, and I was feeling some better. Randy was bowling in a league that night and I was going to try to meet him about 8 pm to eat supper for our anniversary with him and some friends. At this point I hardly ever went out alone but I wanted to meet them. I was getting myself ready, switching from my concentrator to the portable O2 tank when the phone rang and it was my transplant coordinator, Brenda. She asked how I was, how I was feeling, had I had any fevers in the last few days, and was I alone. I told her I was doing ok and yes, I was alone. She said, “I think we have some lungs for you if you are ready for them”. I was shocked! They told me I wouldn’t get this call for a year and a half at least, and it had only been about 7 and a half months…….!!!!!I told her YES, I was ready for them! I was crying by now… she told me to calm down, and how long would it take us to get there. I told her I thought an hour or two at the most, she said that was fine. I called Randy and he was home in minutes. I called my family and a few friends. I was feeling every emotion in the book and thanking God, and already thinking about my donor and the family. I was crying, laughing, nervous, etc, etc, etc!
As it turned out, the reason I got my call sooner than expected, was all a strange situation and a miracle. There is a little confusion about this but I remember being told and my family also remembers being told that I was not first on the list for my blood type (A) and lung size. A terrible thunderstorm northwest of Norfolk was going on (terrible as in, torrential rain, lighting, wind, etc). We were told that there were actually 2 others ahead of me on the transplant list. One potential candidate had some complications going on which excluded him/her from being transplanted at this time. The other candidate was in an area a few hours into the thunderstorm area, and they declined because of the weather. It seemed almost like those lungs were destined for me! It turned out that they didn’t do the surgery that night. My donor was “in house” at the same hospital I was at and still on life support, and with the storms, the doctors from other hospitals were also having trouble flying into Norfolk to retrieve the other organs. So I was admitted and had a fairly good nights sleep and everyone in my family went back home except Randy who stayed with me. They were all back bright and early the next morning.
Marginal lungs???……..Dr. Quaranta, one of my pulmonologist’, came in early and had a very frank talk with all of us. The lungs had started to deteriorate some. Did I want them?? They weren’t in great condition and not what they had expected, They called them “marginal”, however they still felt they would be ok. If I did not take them, and took a chance on waiting, I was in such bad shape, they said, you may not “make it” for the next set of lungs. They felt I should take them… at least I would have some chance. If I waited, I may have no chance, however they knew this had to be my decision. My sister later told me if this had been her, she would have been hysterical if she had been told this and had to make that decision. You would think…. What a decision! I talked briefly with my husband and family and they felt I had come this far I should go ahead with it, as I agreed. I had my mom on my mind and asked my brother what would she tell me to do and he said she would say to “go for it” (and I knew too that is what she would say). So when my doctor came back in I said “let’s go for it, I am ready!!” And I was… like I had said the night before, I wanted something to happen one way or another, because I was tired and didn’t think I could continue the same way any longer. Although I guess I was still very nervous, I didn’t really feel scared. I was realistic however that I may not make it through the surgery, but I was at peace that what ever happened was God’s will, and I would be ok. I remember my coordinator giving me a pep talk right before I went in, that things were going to be fine! My family and I, and my husband said our good byes and “see you soon’s”. It was very emotional. My sister was saying scripture as they wheeled me into surgery…. “The Lord is my Shepherd….”.I remember going into the OR and talking briefly with a few of the nurses and docs and then I was off to la la land !
The Surgery and Hospital Stay
That was May 20th, 2000 a little after 10am. My family was updated throughout the day. They were told I was put on the Heart/Lung Bypass machine during the procedure. The doctors finally finished up about 9 hours later. They came out and talked to my family at about 7:15pm and were very pleased with how things had gone. My sister later told me how pleased the doctors were that everything had gone very well. She expressed how she could see and feel their genuine elation. She said they seemed as excited as if the had just won the Super Bowl! The next thing I remember was waking up surrounded by my family… I thought this was maybe the next day…. well no, it was 6 days later, May 26th. They had me in a drug induced coma for various reasons. I remember coming to a little and everyone talking to me, with their masks on, and me trying to talk to them, and everyone was very happy. They told me how well I was doing. I remember Randy, my husband, was not in the room but outside waving at me through the window and giving me the thumbs up sign. They told me he had a little cold and the doctors thought it best he not come in since I was so highly immuno-suppressed at this point. I also remember the walls of the room looked like it had spiders on it, they assured me it didn’t! The medications were causing me to hallucinate. Everything seemed like a fog. (I remember only bits and pieces of the next couple of months and most of what I am writing now is based on what I have been told from my family, my sisters journal and the tx team and doctors.) I’m not sure but I think they had taken the ventilator out at this point (according to my sister they took it out on the 26th when they brought me around), but it didn’t stay out long at all. The next thing I really remember, only very vaguely, if at all, was on June 1st, them telling me that I had some coagulated blood surrounding my lungs. It was keeping me from progressing and was causing me problems and they were going to have to take me back to surgery to remove the blood. They opened me up again in the same scar as when they did the transplant. They suctioned a lot of blood out, by going down through my ribs. They didn’t have to open my ribs up this time. So here I go again, trying to recover from surgery #2. At this point, I still had not even been out of bed since I went in for the transplant on May 20th. After the surgery I was very restless and couldn’t concentrate. They said I was having hallucinations due to some of the medications and I remember having really strange and realistic dreams. I was just generally tired and weak and restless and it seemed a zillion IV’s and treatments. They did take the vent out again at some time during this period, I think for a day or two but I was not doing well and they put it back .Physical and Occupational Therapy began working with me again going very slowly. Physical Therapy was just getting me to sit up on the side of the bed and had to physically lift me to a chair to gain some strength by sitting up. When they did try to get me to stand that first few times, my body would not cooperate. As much as I wanted to stand and “do good” I couldn’t. My knees felt like they had cinder blocks on them. They would just buckle. My ankles and knees were swollen huge. Even my eyes were swollen. At this point, they just worked mostly on exercises in bed, to try to help me gain some strength so I could work up to standing. I assume I was so weak during the recovery process because I had been extremely weak before the transplant and then ended up with the second surgery on top of the transplant. Occupational Therapy had me trying to do things like brushing my teeth, or holding a washcloth to wash my face. This was all very hard on me…. I had no idea how fast I would lose all of my strength but they reassured me that I was doing “great” and encouraged me to keep trying. I felt like a baby learning to do the simplest of things again. If not for my wonderful support system of my husband, family, friends and my doctors and nurses (my nurses and therapists were like angels….I never had a bad one) and all the encouragement they gave I am not sure I could have mentally and emotionally made it through this period. (My hospital has a few guest suites upstairs on one floor for out of town families to stay in for $15.00 a night. It is a regular room with a bathroom. My family rented one of these rooms early in my stay and kept it almost the whole time I was there, so one of them, be it my husband, brothers, sister, sisters in law or a friend, could stay and be close at hand at all times. My brother Marvin was there so much I think everyone at the hospital knew him. They still had to abide by most of the visiting hours in ICU but my nurses and doctors knew they were always somewhere around and it was very comforting to me because I became a big baby and wanted someone with me as much as possible). It would have been so easy to give up, but I was stabilizing well and they moved me to a step down unit I think on June 5th, just 5 days after surgery #2.I do remember the day they moved me to the step down unit. I had gotten so used to my wonderful nurses in ICU and I was afraid to move, but I did and my brother Woody was with me for support when they moved me. I was very nervous and anxious, but tried to be positive that this was a big step, showing I was progressing.
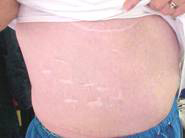
That first night in the step down unit, something happened. As I was told, a very observant nurse, Maria, recognized that when she did my IV’s in the middle of the night, I was not just sleeping soundly, I was out! She tried to rouse me and I couldn’t. From what I can understand, my CO2 level had risen to an unsafe level and I became unconscious. My brother Woody was upstairs and they called him down in the middle of the night. My understanding and from my brothers’ memory of it, is that I was very critical for a while and things did not look good, but thankfully they stabilized me. Woody called my husband and other family members to tell what was going on and that I had been moved back into ICU and back on the ventilator. One of the wonderful Respiratory Therapists, Steve, later told me, “I spent almost the whole night with you trying to keep you alive”. Again all of this is not really clear to me but it seems that it was determined that the CO2 problem arose from a Yeast-type fungal infection that was surrounding my pleural cavity. They worked a while (a few days??) trying to resolve this in several ways. They were placing and replacing chest tubes to try to drain this infection, however this was not working. (When I look in the mirror now, I count 13 chest tube scars. This view is my right rib cage area with 8 scars. Looks like a shark bite!) I really remember nothing during this time except tiny bits and pieces, like frames of a movie. So around mid-June, here we go again, Surgery #3 took place. They decided it was crucial to open me back up again to physically remove the yeast from around my lungs. It was keeping me from breathing on my own and progressing. And (at some point in here) I also developed Sepsis (which is a blood infection that is often fatal), staph and pneumonia related to all of this. I was not well at all. (Later when I got home I looked up Sepsis and had a much better understanding of all that was happening to me.) They did the surgery, opening me back up in the same scar and this time opening my ribs up again. They removed a liter and a half of yeast.
The next day, they did a tracheotomy and also put in a stomach tube, as they felt my recovery was going to be very slow at this point with so many infections and complications going on. They put the trach in so I could have the ventilator in my throat instead of my mouth. I’d had the vent for so long. The transplant team thought any longer may cause damage to my vocal chords and a trach would be more comfortable for me.
In my sisters words in her journal she was keeping she said. “Things were not looking very optimistic “.However, from what I remember, everyone was very positive to me and kept rallying around me. I still don’t remember much, except it seems I fell asleep and when I woke up I had another surgery, and a trach and a feeding tube. At some points, I think they put me back into a drug-induced coma. Every time I would wake up, I didn’t know if I had been asleep for an hour or a few days. My mind was mush! It was hard for me to stay positive but Lord knows I was trying too even in the state of mind I was in. Again the meds were playing havoc on me, I was still hallucinating and having really strange and bizarre dreams again, that seemed so real. I was having crying spells, and at times resisting care. They had to suction my lungs a lot. At times I didn’t even know why I was in the hospital and was begging my family to please let me just go home. I couldn’t see much progress but they insisted I was making progress. Physical and Occupational Therapy started working with me all over again. I was right back to square one. I wanted to get better so bad, but Physical Therapy was soooo hard. I cried everyday on and off. I was so weak and tired and they kept telling me “you can do it!” Sometimes I thought it would have been so much easier to just give up, but something made me just keep trying. The nurses and docs and my whole team, and everyone were just so encouraging to me. Dr. Garnett and Dr. Quaranta were there to see me every single day, sometimes several times a day. Everyone told me about all the prayers for me… people I didn’t know, churches I didn’t know, friends of friends all over the country… it was overwhelming… I never realized the magnitude of what was happening (and the power of prayer).
On July 4th, I was paroled from my ICU room for a little while. This was the first time, other than for a few tests that they had to take me out of the room for. From some areas of the hospital you are able to see the river where they do annual July 4th Fireworks. I was having such a hard time emotionally that some of the nurses along with my family asked the docs if they could take me out to areas of the hospital so they could let me watch some of the fireworks through the windows. I would be on my machines and in a special cardio-chair that you are kind of sitting up in, but not a wheelchair. They felt I needed the change of scenery if only for 30 minutes. To do it some of the nurses had to come back that night on their time off because it involved too much for the regular staff to do to get me up and out and not neglect the other patients. That staff was so wonderful… 3 or 4 nurses and a Respiratory Therapist all came in on their off time to make sure I got to do this. It was wonderful to get out of my room on a “pleasure trip”!!
I was difficult to get off the vent, because I was so weak, had infections, etc. When they tried to wean it off I struggled to breathe. The docs told me “we will take this slow because we know how weak you are” and it took a few weeks to wean me off of the vent and build up my lungs. They would cut it off for an hour one day, then 2-3hours, then 4-5 hours, etc. until I was off for most of the day. As I was being weaned, I would become so tired and worn out after a few hours off of it, however it was the only way to wean me off and get my lungs stronger. I also had the trach so there was a lot of sign language and charades going on in my communication. I was trying to write and my hands were way so shaky from medications and weakness. My family and I found that a sense of humor is good to have in times like this. Sometimes when I was trying to make them understand me I was laughing and crying at the same time! They eventually were able to start using a “pasa muir” valve with my trach, which the nurses would put in when I had company or docs were in so I could ask questions. It was much easier to talk with this in but I could only keep it in for short periods. I also gradually started eating some foods, even though I still had tube feedings. My nutrition was so poor. I am told I was at 89 pounds at one point (and I am almost 5’9″ tall). I was also having stomach problems. I had trouble keeping foods down for a while and also had diarrhea. Physical therapy was progressing slowly but surely. I really believed at first that I would never walk again. I was finally able to take 2 or 3 steps to a chair, with lots of assistance. Each day was a struggle and a victory at the same time! For a while, I cried every time the therapists would come in, but I new it was necessary. It was such an ordeal, and they were so persistent!
Around mid July, they finally had me off the vent and some of my other problems were stabilizing, I was able to move back to the step down unit. Moving out of ICU made me very anxious again after realizing what happened the previous time I moved out. One of my best friends, Kelly, was with me for the move for support and to help relax me. I had gotten so comfortable with the nurses and routine of ICU, it was really scary, however once there I seemed to progress much better. I still was using a little O2 but finally they made me give it up even though I thought I needed it… I didn’t! They even had been turning it off at times I thought it was on. I remember so well Dr. Quaranta telling me they were going to stop the O2 and my little protest with him about that! I started walking with assistance and a walker to a chair or to the bathroom…. Oh it was soooo hard and each step was like a victory. I was trying (sometimes unsuccessfully) to be “upbeat and positive”. I wanted my family, hubby and or friends with me all the time. I was still being a baby!
Some of this period is still vague to me, but things were starting to come together and looking brighter. I was able to eat a little better and I could see progress in areas like walking, strength, and endurance. They took my trach out near the end of July and worked on getting the opening in my throat closed up. This seemed like a real step to me! My voice was very soft but was improving. They stopped using the feeding tube and I ate regular food but they kept the tube in just in case I needed it. Respiratory Therapy was still doing nebuliziler treatments several times a day to treat the lung infections.
I think it was around the first week of August when the transplant team felt I was stable enough to work more on getting my strength back full time. They moved me upstairs to a total rehab floor. I still had my doctors visiting me often and still had Respiratory Therapy coming and doing treatments daily, etc. I was told they would work me hard… and did they ever! I still weighed less that 100 pounds. I think I was there about 3 weeks, with very intense Physical Therapy and Occupational Therapy and also Recreational Therapy (which is the field I was in before I got sick…I was getting a dose of my own medicine!). I was finally starting to realize my new lungs were really working and it felt good! It was a good, positive experience and I worked hard and I was worn out every night. Reesa, my Physical Therapist was great and was very serious about getting me walking and stronger. The picture on the left is my last rehab session, the day I went home, and the right is my coordinator, giving me last minute instructions. While I was in rehab, one of our concerns was that my insurance was nearing its million dollar cap. A miracle then happened, my insurance company changed companies, and when they did, my new insurance started back at $0 . When I left there on Aug. 23rd for home, I was walking with a walker or cane and had no oxygen. I had been there for right around 100 days. When I left there on Aug. 23rd, it was exactly a year to the day of my first visit with Dr. Burke, when he told me I needed a transplant. What a year! It was so overwhelming and emotional to be headed home. Even though the last 3 months had not been what I had planned, I thought of all the wonderful people I had met, how this had brought me so much closer to my family and how this experience had changed my life in so many ways! I thought,”Ok…now I can get back to living!!
Finally Going Home!
I came HOME! I was very positive that things were going to get better and I was on my way. Well… it wasn’t exactly like that, it just wasn’t in The Plan. My sister, Nancy, stayed with my husband and I for a few days to help us get things settled and to help me out because Randy was working during the day. I was getting rehab and things were going slow but ok. A couple of weeks after I got home I ended up back in the hospital for a few days. I believe that first time was some problems with medication levels playing havoc with my stomach. I was going to clinic weekly for a good while. Soon it seemed I would go to clinic and every month or so they would put me in the hospital for something. I got a bad blood clot in my left leg (that still has not totally gone away), medication induced-diabetes, medication levels off, shingles, stomach problems, a pseudomonas infection, fungal infections, and I was having brochoscopies done every few weeks (or more at times).
Every time it seemed like, “Ok, I am on the right track now”, something else would happen and I was getting very discouraged again. I was going to out patient rehab but all these “things” were coming up, making it hard for me to really get motivated, although I could see I was getting some stronger and I was gaining some weigh back slowly. I was getting around fairly well, but my stamina and endurance were still very poor. I was still very shaky from both weakness and medications. By December, I was on home IV’s for a very serious fungal infection, with Home Health nurses here everyday for several hours. I had done some home IV’s before and they taught me how to do them myself. They are pretty easy, but for the fungal infection, I was on one really powerful IV that required nurses to observe you and administer it daily. I had a difficult time with it. Everyday while taking it I would get sick in my stomach. They had to come to do one of the IV’s and I was able to do the other ones on my own. Next, the IV meds were dehydrating me, so I also had to do fluid IV’s at home which they taught me to do with the IV pump all night. Between all the different IV’s, I was on IV’s more hours than not during the day and night. One of the meds they gave me with the IV’s would make me sleep almost as soon as I took it. Also, I doing nebulizers twice a day. Emotionally and physically this was draining me. I had to stop rehab because I was on the IV’s so much of the day and had to work around the schedule of the Home Health nurses. Again, I lost a lot of what I had gained. I was not able to get out much at all. The Home Health Nurses were wonderful but it was almost like they lived at our house. Between IV’s and dressings on my PICC line, teaching me how to do the procedures, and they were doing some blood draws, besides still getting use to managing taking between 50 and 60 pills a day, once again I was overwhelmed. During this time, I also had to get use to giving myself insulin shots daily and also Heparin shots in my stomach, because of the blood clot in my leg. This was all hard on my husband too. So many new routines, Home Health Nurses in our house at all hours, little privacy, etc. This was a difficult time for us. I kept telling my self, things have got to get better. My family and husband were making so many sacrifices for me, and I did not feel worthy of this. I was really pretty dependent on them still. I was very trembly from some of the meds, and still not strong enough to drive. I was just struggling to keep going from one day to the next, and trying to keep my faith that there was a reason for me to go through all of this. I don’t know what it looked like to people on the outside looking in………..maybe they thought that I was giving up and not trying ???But to me, I was struggling to stay upbeat and positive and just get out of bed everyday, but it was not an easy job some days. I really was having trouble staying motivated because it seemed every step forward resulted in two or three backwards but I was not about to give up. My goal for each day was really to make it through another day and some days that was easier said than done! Nevertheless, I still believed that better days were coming. It is so hard to describe how I was feeling at this time.It seems to be one of those situations that you never really know how someone feels unless you have been on a similar situation. You can empathize but you may never fully understand.
This was also the time I finally started to grieve about the loss of my mother, which happened just before my transplant. I was so sick when she died that it seemed I just went through the motions. Now I was feeling just how much I missed her. She was so wise and seemed to always know how to handle things. So many times I just wanted to sit and talk with her and ask her how to better handle what was happening to me. I was having way to many “pity parties”. Often I would think,…. I lost my career and job of 17 years that I loved. I lost my health, my independence and my parents.I didn’t even look or feel like the person I was, I was swollen and bloated and my hair was falling out and thin from meds, and at this point it was beginning to look like I might lose my marriage also. But then I would try to turn things around and say BUT, I AM ALIVE!
This was very stressful and painful for us all, this type of situation is hard on a marriage and it was showing. Jan, Feb, March of 2001 was difficult because of the IV’s and nebulizers and everything else. I was just overwhelmed. Some of the IV’s stopped in January (I think) and some lasted longer. Those IV’s I was on seemed to wipe me out of any energy and strength that I had started to build the first few months after getting home. I felt like I was spinning my wheels and going no where. I still couldn’t drive, I was too weak and shaky, and my eyesight was failing too, so I was still dependent on others to take me to doctor’s appointments, or anywhere I needed to go. I was trying to do more for myself and gradually I was starting to cook more and do things around the house but I was still taking baby steps. Everyone was so patient with me, encouraging me to start doing more and pushing myself more. I really felt at the time, I was doing the best I could for myself.
Around April, my husband decided that it would be best for “us” and for me if he left for a while. It was a difficult decision for him. There had been a lot of stress for some time. It was mostly things related in one way or the other to my transplant. He was frustrated with me and felt I was not trying hard enough and pushing myself to get better. It seemed an unconventional way to get me motivated, but he used “tough love” on me, trying to motivate me to try harder and get back to my life. He moved in with his parents but he remained very supportive. He came over everyday when he got off work and checked on me, usually we had supper together and he would stay for a few hours and then leave. I felt I was doing all I could do, all my body would let me do, but at that point I realized I needed to start setting goals, even if they were small ones. I started walking to the mailbox … then one house down, then two or three houses. I had been trying to exercise for some time but the complications kept hampering me. Just a few days after my one-year transplant anniversary, May 20th, 2001, I was back in the hospital. (During my first year, besides the first 3 month+ stay, I was in the hospital I think about 6 or 8 more times. I knew all the hospital routines, the nurses, x-ray techs and housekeepers by name, and what meal was served on which day.) This time it was a mycobacterial infection, another fungal infection, and problems related to meds. I had been looking so forward to attending my nephews wedding at the end of May. This would have been my first big event since my transplant. I was looking at it like a “coming out” party, but I was in the hospital, again. This again, was very disheartening to me, but my overall out look was getting better. I had set short term goals on exercise and walking and I told one of my doctors, (Dr. Burke, who had diagnosed me and told me I needed the transplant) during that hospital stay that my long term goal was to climb the Cape Hatteras Lighthouse again one day.
I was serious too. A few months earlier, in a talk with Randy, I had wondered if one day I could climb the lighthouse again and now I was determined to do it! The Lighthouse was a symbol to me. It had weathered many storms and people thought it was going to fall but it didn’t and hasn’t. I felt in some ways like that Lighthouse… I had weathered many storms, and some people thought I would not make it but I was still standing (although wobbly) and planned on remaining standing.
Back Among the Living!
When I finally got home from that hospital stay, I took a huge step and made a big turn around! I realized that everyday is a gift that I wanted to enjoy. I was tired of sitting around and watching the world go by without me. I had not come this far to sit around. I was ready to reclaim my life! My life had been running me, I was going to begin to run my life! My doctors had told me the first year is often difficult, and how right they were. I was just a little over the first year point now. I was on and off of home IV’s again, because of the infections. As I gained strength, (and I really was gaining strength and weight) I felt like I wanted to start driving again but by now my eyesight was failing badly. I went to the eye doctor and I had nice big cataracts in both eyes, caused by the prednisone use. My transplant doctors didn’t feel I was ready to go through cataract surgery yet. So I was having yet another test of patience. I was living alone still and doing better but anxious to start being more independent. With not driving I still had to depend on others for a lot of things. My family and friends were a Godsend.
I was doing better all summer and progressed to walking a half a mile, a mile, two miles and more!! My husband got me a bike and I started riding everyday. I was getting stronger! Even though I was doing home IV’s still, I was feeling more confident and really feeling good physically. Although during all of this I felt I had been fairly positive considering how bad things seemed at times, during this period I really took another big step forward in attitude and motivation and just staying positive. They finally let me have the cataract surgeries, one eye in August and the other in early September. That was another BIG step and I soon began driving again for the first time in about 16 months. I felt like a bird out of a cage…watch out world, here I come!!!!I started bowling again in the league I had bowled in before I got sick! It was a combination of therapy (I was looking for all types of fairly simple exercise, not overtaxing, that I was capable of) and socializing. I finally regained some more of my independence …. yeaaa!! On Sept. 11th, the morning of the 9/11 bombings, I had a permanent Greenfield filter put in my vena cava .I still had blood clots in my left leg and was on Coumadin, a blood thinner. The blood clots were getting smaller but being stubborn about going completely away. With the filter I could come off the Coumadin and not worry about the clots traveling if they broke up, which could be very dangerous and fatal. The filter would catch them. That was a weird feeling being “put under”, just after watching on live TV, the towers being hit, while in a waiting area with my brother Marvin, as I was being prepped for the surgery. I made out fine with the surgery.
After that, I began to really feel myself improving more. I was moving around better, and increasing my stamina and endurance, and doing lots of new things! I still had that chubby “Prednisone face”, as I call it! That’s me and my niece, Jomie, at her wedding shower I was taking one day at a time.I still was doing a home IV in my PICC line (I think 3 times a week?) With the blessings of my doctors, I started an exercise class two days a week at our local Parks and Recreation center, that included low impact aerobics and weigh training (I was very careful with my left arm with the PICC line, but could still exercise). I was still walking and/or bike riding a couple of miles almost daily … religiously! (I had done rehab on and off but with all the hospital stays and home IV’s along with me not driving, it made it hard to keep it up. I had started my own rehab program in a sense, with the walking, riding, etc.) This was another big step. It was actually a Senior Citizen low impact class., but they cheated and let this 42 year old in ! . It was hard but I never missed a class unless I had an appointment… no matter how bad I didn’t want to do it… I did it! I treated my walking and riding and exercise classes as if it were not an option. It was just like my medicine, something I had to do to get better and stay better (and I still have that attitude about exercise). I didn’t wake up in the morning and think, “Do I feel like it?” I woke up mornings thinking “I don’t feel like doing this but I have too do it!” Then and even now, if I don’t feel well in the morning, after I go and exercise I usually feel a lot better. I was getting a little more adventurous. My husband and I went to a Redskins football game in Washington (just 4 hours from us) and that was a great weekend. Next my husband and I were going to Busch Gardens and I asked my docs if it would be ok for me to ride the roller coasters that I love so much. They said, ” Sure, go for it!” And I did and it was GREAT!! That’s me on the back row on the right with Randy, with my hands in the air and with the Don King hair style!!
People were seeing me and surprised at how much better and stronger I looked. Although I had faith that God would bring me through this, I really was surprised and proud of my own progress and just how good God is!!!I also was having some guilt feelings… I had come through all of this, I felt for a reason… and I wanted to know what that reason was, such as, was there a duty I needed to fulfill? But again, I began feeling like if there was something God wanted me to do, he would show me in His own time.
By the beginning of 2002 I was doing very well for the most part. I was still on some home IV’s for the mycobacterial infection, but was able to administer them myself. However Home Health nurses still had to come by every few days to change the dressing on my PICC line. My life was pretty busy again for a change. Between all of my doctor appointments, (Lets see – there was the stomach doc, diabetes doc, vascular doc, eye doc, transplant docs, GYN doc, Dermatologist, labwork, etc.) and the normal routines of a transplant patient (home IV’s, meds several different times a day, insulin, checking blood sugars, doing daily breathing tests on my home spirometor, I could go on!), and going to exercise classes and errands I was always ready for a nap when I got home every afternoon. My doctors were clearly pleased with me and Dr. Garnett told me, as the saying goes, “You’ve come a long way baby!”
I came off all IV’s in January 2002 I believe. My life seemed back on track in most areas. I was not on any IV’s or antibiotics for the first time in a long time. I was down to taking 30some pills a day instead of the 50 or 60 or more I had been on at some points during my recovery. My breathing tests were steadily improving. Life was good and I was really starting to enjoy life to the fullest again! And I was still looking back and thanking God… for sustaining me, and asking Him to help me keep improving and moving forward, because I wasn’t done yet! I still had goals to reach! My supportive and loving husband was still not living at home with me, although we had remained very close, seeing each other on a daily basis. In March he decided to move back home and I was thrilled!!
For most of 2002 I had very few extenuating health problems, just a few minor things that are normal for transplant patients. I was still learning to manage my time, my health and regain my strength. I was in transplant clinic every couple of weeks for tests, lab work or breathing tests. My transplant team is so cautious (thank goodness!) that any little thing that comes up they want checked out. Little things did come up but nothing too serious. I felt as if this was a breeze compared to the whirlwind I had been through before and since transplant. I was well enough to drive myself to Norfolk for my appointments and I could do most things on my own again. The fall of 2002 I added two more days of exercise to my schedule. This was a harder class. It was faster paced aerobics (but still low impact), and included weights, floor exercises and sometimes some yoga. The floor exercises were really challenging to me because I still had trouble just getting on and up from the floor! I couldn’t (and still can’t) always keep up with the others but I give it the best effort I have! Without the exercise routine I developed, I really don’t think I would be doing nearly as well as I am. My doctors tell me my breathing tests are so good because I give my lungs a good workout with my exercising. I was doing more and more all along. My husband and I had been back to surf fishing for a while, but I finally tried off-shore fishing again, which I had not done in while. Talk about testing those muscles!
(The scales and skin of fish carry bacteria, so when we fish, I do not touch the fish until it is cleaned, unless I am wearing gloves. Just one of those precautions my transplant center asked me to take because of my compromised immune system. Randy cleans, I cook! Also, another precaution I must take is plenty of sunscreen when outside. Transplant patients are extremely susceptible to skin cancer due to medications we take.) 2002 turned out to be a great year! It was a year of rebuilding, renewing, regaining, recharging my batteries and learning my limits. In early 2002 I finally stopped my IV antibiotics and nebulizers. I had some problems come up which are expected with any transplant patient such as medication levels getting out of whack, diabetic problems, restrictions related to being immuno suppressed, tiring easily (still needing that daily nap it possible) and learning to pace myself, etc. But, these are simple things that I can handle. My motto is “Don’t sweat the small stuff”, and all of that is small stuff.
In the spring of 2003, I had not forgotten the goal to climb the lighthouse and I felt I could accomplish it soon. I increased my exercise, to include walking several flights of steps several times a week. I knew that I could achieve that goal one-day. The Lord had walked a long way with me over the last few years, carrying me a lot of the way, and I knew He would be glad to walk with me to the top of that lighthouse. That lighthouse is like my kindred spirit, there is a bond that others may not understand. On May 17, 2003, I finally met my goal! I, along with my husband and a couple of friends walked up the 12 stories to the top, almost three years to the day, from the day of my transplant. It was a thrilling, exhilarating and spiritual feeling to reach the top. I felt like Rocky at the top of the steps! I had to stop and rest a few times on the way up but that didn’t matter. That lighthouse and I have both weathered many storms but neither of us let them defeat us! I hope to make climbing the lighthouse a yearly ritual to celebrate my struggles and my accomplishments! To the left below, is our fishing trip off Hatteras , NC , July 2003. What a view of the ocean from the bridge of an off shore boat!
Despite all we have been through the last few years, my family and I feel like our lives have been enriched in many ways by the experiences we have had. I have never felt bitter or “mad at God”, as I sometimes have heard people say when they experience struggles. I think the struggles have made my life better! I have had the chance to meet so many wonderful people that I would have otherwise never met. I have found that as you go through hard times in your life you learn to appreciate the beauty in life and in people, and in everyday things. I am on several different groups on the Internet and have learned so much from so many wonderful people I have never even met face to face. I hope that in some small way I am helping others too. Once I saw that God was going to keep me here awhile, I had to decide if I wanted to live or merely exist. I am choosing to LIVE! By my story I want others to see that obstacles get in our way and things don’t go like we had hoped or planned, but we can’t let them get the best of us. God never told us that life would be easy. We can overcome the hard times through prayer, determination, patience, positive attitude and pushing ourselves even when we don’t feel like it or think we can! One of my favorite sayings is “Life gives us blessings and hurdles, you have to count your blessings and jump your hurdles!!” and another one of my new favorites, “Even if you are on the right track, if you just sit there you will still get run over”. I don’t know why God left me here… I do know that prayer had a lot to do with it, and that it was His will. I do feel He has a plan for me and I hope that I can fulfill it.
What is sad to me is that as I live on, someone died and that family is missing him everyday. I thank God daily for giving that family the strength, generosity and love of their fellow man, to donate his organs at such a difficult time for them. The donor and his family are the heroes here. I know that he was an 18-year-old, who had a traumatic accident. Although the hospital was not able to tell us much more than that, I have learned more about him through other families that my family met while in the waiting room in ICU and also via newspaper articles. I have written one letter to them, about a year and a half after my transplant. I wanted to write earlier but I was having such struggles. I decided to wait until I had good things to tell them about how I was doing. Unfortunately, I have not heard from them. Everyday I wish for a letter from them in my mailbox. I plan on writing another letter soon. I would be so honored to meet them or just talk to them. I know it would be difficult for them but I would love to try and express my thanks to them, and show them that in some ways their son is living on. Near the 3rd anniversary of my transplant I placed flowers on the altar at my church in memory of him and did a talk about the experiences I have had. I hope in some way I am promoting the importance of organ donation by being a living example of the success of transplantation. I have been to meetings at LifeNet, the organ procurement agency for my area. I am hoping to get involved in some Donor Awareness programs, but already I do a lot of one to one donor awareness with people I come in contact with everyday. I feel that others are more apt to consider being a possible donor when they see transplant recipients having good outcomes and experiences.
This has been a challenging but good experience. It is not something I would choose, but I feel it has made my family and me better by the experience. Although sometimes it was tough, and sometimes I lost faith in myself, I really kept my faith in God all along, and still do. I know that He will do what is best for me and I trust him. I really hope to stay here a while longer but I am realistic, and know that things can change so fast. I recently lost two dear transplant friends. This was very hard for me to except. Both of these friends had been doing well just months before. I plan on being here for years still, but then, I’m not the Master Planner.
Trying to Stay Healthy and Well While Living With A Chronic Health Condition
Many people assume that when a lung transplant patient is doing well and looking healthy, that their life goes back to “normal” (what is “normal” anyway?).People look at you and say, “Well, you don’t look sick.” Speaking only for lung transplant patients, and really myself, I can tell you, your life is never “normal” again after a transplant, especially if you plan on staying healthy, well and out of the hospital. I am not saying your life is not good, my life is GREAT, and very worth it, just not “normal” based on what most people perceive as “normal”. When living with a chronic illness or condition, there are so many things to be considered that many people, even the doctors don’t realize or understand. Almost every single thing you do has to be thought out, often ahead of time (the type of things that others don’t have to think about at all). Some examples of this are: you can’t just sleep in late whenever you want, because you can’t miss your meds. You have to plan your day out somewhat, because you have to consider when and where you will be when you have to take meds, insulin, etc. You may decide at the last moment you want to do something with a friend, but if I already have plans later in the day or the next day I have to consider my energy and stamina. When going to an event, you have to consider will you have access to water for meds if you can’t take your own water. Also, when going to events or gathering you have to consider how crowded and in how close contact you will be with others, to decide if a mask may be necessary, especially during flu season or if kids are involved. When going to visit friends, I often get there to find that they forgot to tell me they or one of their children has the flu, a bad cold, etc., so we very politely leave or only stay a few minutes. When traveling, I have to make sure I have plenty of extra meds as you never know what may come up and delay your return. Also, when traveling far from home, most transplant patients are smart to look at hospitals in that area that are familiar with lung transplants patients, just in case. When I go watch my husband play softball or I am outside for other reasons and it is windy, I sit downwind of the dust or try to get out of it, or use a mask. The dust and dirt carry fungus that would not effect a normal person, but can and often do, give an immuno-suppressed person an infection that can be very severe. (The worse fungal infection I had was thought to be from road construction dust near my house.) If I want to plant flowers, my center asks that I wear a mask and gloves. I could go on and on! I am not saying these things to complain at all, just to make you aware that the fact that I have a chronic health condition is at most times on my mind, as is most likely the case with other transplant patients. I try to not live in a “bubble” but just use common sense. I try my best to stay healthy and well, which is the best way I can honor my donor and his family for the gift they gave me. I have found that to keep myself well and healthy, I have to maintain a great degree of self-discipline! The main things that I see that I must do daily and keep in the forefront are:
1) Keeping my medications extremely accurate every single day. Not keeping them accurate would be detrimental and is a matter of life and death. Managing taking around 42 pills a day is not a simple task, although you do get use to it. They have to be taken on time every day, especially the anti-rejection meds. I have to consider which meds may interact with the others, which need to be taken with food, etc., so I have several different medication times to remember throughout the day and also insulin. I take pills at 6am, at breakfast time, at 9am, insulin about 11am, pills at lunch and mid afternoon and at 9pm. This is my pills for one day A few have been added since this picture.
2)I am extremely cautious about being around germs, infections, bacteria, viruses, fungus or anything that could make me sick. Since my immune system is suppressed (not working properly) due to my anti-rejection medications, a simple cold, or infection that would not even phase someone with a normal immune system, may end me up in the hospital or worse. When I go to doctors offices or hospitals I usually wear a surgical mask, as do most lung transplant patients (and is recommended by my docs), to protect me against germs and infections of others. I have a whole new mindset when it comes to germs, I am always conscience of them. When I shake hands, with someone, or touch a grocery cart or a doorknob, it is not long before I wash my hands or pull out the Purell. Dust, soil, mold, mildew are all things I am very careful around. Transplant patients learn pretty quickly what to avoid, or what to wear a mask around. Germs are in places I had never thought about before my transplant. You have to learn to use common sense. If you do that, you can find ways to do most things without feeling like you are living in a bubble.
3) I need plenty of exercise and activity to help keep my body strong, help my cardiovascular health, help control my diabetes, help maintain my weight and help to ward off depression.
(Many transplant patients are on anti-depressants because many of the meds can cause depression. The complexity involved in keeping up with everything can be very overwhelming. I have been on anti-depressants, but I am not needing them at this time. I do have an anti-anxiety med I take if needed.) Many of my medications cause side effects that I have to deal with everyday, including hypertension and possible heart problems, diabetes, swelling, shakiness, stomach upsets, along with many other side effects that exercise can help to offset.
Prednisone especially weakens bones and muscles and the exercise and use of weights helps me to loose less bone density and muscle and helps to maintain what I have. I go to Parks and Recreation exercise classes usually 4 days a week unless I have an appointment. If I have to miss exercise classes for more than a day or two my body feels the difference. I also take walks, ride my bike and bowl on a regular basis. I try to see that I have some type of exercise type activity daily. Even with the exercise I am still pretty weak, especially my legs.
4) Preventive/Proactive Healthcare….I make sure I drink at least 2 quarts of water a day, at a minimum. Many of my meds are very hard on the kidneys and this often becomes another big issue with transplant patients, sometimes leading to dehydration, kidney failure, dialysis, kidney transplant or death. My doctors tell me one way to help avoid this problem is by drinking a lot of water, although that is still not a guarantee (I have learned there aren’t many guarantees in life). Usually if you see me, you see my water bottle! Also along the lines of prevention and being pro-active, I have a Home Spirometer which is a portable machine that can test my breathing and can be an indicator that something is wrong. If my “numbers” start to fall, I would call my doctors, as this is usually an indication of rejection or some type of infection or problem. I am very in tune with my body. The slightest little thing “different” or wrong can easily turn into something big, so I try to always be aware. I call my coordinator any time I am unsure or have a question about anything and they always follow up. I always follow my doctor’s orders. I have come too far and they have put too much effort and expertise in getting and keeping me well to not do what they say. If I disagree with them on something, we discuss it. Although I don’t have nearly the number of doctor appointments or lab work I did in the past, I am still in doctors office or having lab work, or on the phone with an office every week or two if not more. Although they are looking out for you, you have to look out for yourself too!
5)Attitude and Activity! I try to have a positive, healthy attitude about life and about my illness. Ok, I admit, sometimes it doesn’t work and I have a “pity party” about this or that, or feel like throwing a tantrum, BUT I don’t and won’t let myself stay in that “place” or that state of mind for too long. I say, “OK, that’s it, enough of this, pull yourself out of this and put yourself back in a “good place”, a better state of mind.” Staying positive is not always easy, but I have found that being happy is a lot better than being miserable. I have a whole new attitude about what bothers me….. as they say, again, I “don’t sweat the small stuff” so much anymore. So much of what we worry about is just not worth the worry. It helps me to read positive, inspirational stories, poems, etc. and to be around “upbeat’ positive people. I love all kinds of music, and especially songs that speak to me and I can relate to. About a year or so after my transplant a country song came out by Jo Dee Messina called “Bring on the Rain”. This song really spoke to me and still does. I get inspired every time I hear it, so I play it often! It says, “can’t imagine what else could go wrong”, and wanting to “hide away somewhere and lock the door” but eventually the song leads to this may be “a single battle lost but not the war”, “tomorrow’s another day……I might feel defeated, and I might hang my head, I might be barely breathing, BUT I’m not dead!”. This song reminded me so much of myself. At times when things were going wrong, I felt defeated, but it didn’t mean I was giving up. I may have lost a battle, but I was still fighting the war! I also recently bought a little book that was very inspiring to me called, “My Beautiful Broken Shell”, by Carol Adams. Staying active keeps me positive, and being positive keeps me feeling like being active. They work hand in hand. I take a whole day now and then, to do nothing except be a couch potato but these days are few and usually just when my body tells me to take a break and do nothing. I do take an afternoon nap most days, but that is after a busy morning or day of exercise, errands, appointments or working around the house and being generally busy. I have found that my body, my mind and my attitude function best if I get a nap on busy days (not to say that I always get one though). Many people wonder what I do to stay so busy since I am not working. Staying healthy and well IS almost a full time job in itself when you think about it. All the appointments, pharmacy trips, phone calls to my tx coordinator, doctor offices and insurance companies (these calls are never simple, I could write a book on experiences with insurance companies), exercise classes, walking or bike riding, checking my blood sugar, and remembering when to take meds several times a day and insulin, etc. are all very time consuming. I have taken a few computer classes at the library and plan on signing up for some online classes, with my local community college. I spend a lot of time on the computer, especially on my Transplant Support groups, e-mailing, chatting, learning and also hoping in some ways I am helping others, especially those who are having a hard time with “the wait” or those who are going through rough times post-tx. Another thing I do to stay busy and it also gives me a sense of “helping” others is, doing errands for family or friends when I am out daily, or taking people to appointments, who can’t drive to them or need assistance. My husband and I enjoy fishing, going to concerts, amusement parks, going out with friends, bowling league, etc. I definitely still have to pace myself everyday and manage my time so as not to overdo it. It sometimes takes me longer to do things because I take a lot of breaks. My body is not its “old self”, and a really busy day today usually results in “paying for it” or needing to rest more tomorrow. I have to admit I do tire easily and I am not sure if that is “lung” related, medication related or just related to the trauma my body has been through (of course it is not age related!).With so many meds, so many of them have side effects that sometimes catch up with me. If I am on my feet too much it results in really swollen and hurting feet and ankles, and a really achy back. My doctors tell me to pace myself and LISTEN TO YOUR BODY! And I do, I know my limitations. I may have to slow down a day or two sometimes but that doesn’t hold me down for long! And last but not least,
6) Pray and keep the faith! God is on this journey with me, always right by my side!
Quick Medical Summary
*When I got out of the hospital I weighed a little less than 100 (was at 89 at one point when I was in the hospital). Not too long ago I was at about 163 which is the highest I have ever been. I felt that was a little too much, (even though I am pretty tall, at almost 5’9″) plus they had just increased my Prednisone back up to 10 mg daily, which meant more hunger, more weigh gain. I decided right then I was not gaining more and I wanted to lose a few pounds. By increasing my exercise a little and watching my diet closer, I am now about 153. *I am taking about 42 pills a day, which sounds like a lot, but I know some transplant patients that take many more, while others take many less. I do get headaches, leg and joint aches, and bad stomach upsets/aches at times, some of which may be side effects of the medications. *I take blood pressure medication because some of my anti-rejection meds cause me to have high blood pressure. * I have acid reflux and take medication for this, as most transplant patients do. Reflux can be very dangerous for lung tx patients. I sleep with my head elevated because of the reflux. * I have medication-induced diabetes, for which I take pills and insulin. Whenever my prednisone dose changes, so does my blood sugar range and amount of insulin I take. My blood sugar is always highest in late afternoon when the Prednisone is at its highest level in my system and then will drop to normal often late at night. I can see a big difference in my blood sugar on days I do no or little exercise. Differences in my routine and activity lead to lower or higher blood sugar, sometimes making it difficult to predict. I do have instances where my blood sugar falls to unsafe levels, and I get clamy, shaky, hot, so I take my blood sugar at the first hint of this. It is not that unusual for it to fall to 45, in which case I have to get some sugar in me quickly. (Hey, I never complain about having to eat a candy bar!) *My last spirometry tests (which is an indication of how well your lungs are working) showed I had a FEV1 of 86% (of normal), my FEV25-75 was at 110% and FVC was 76%. The FEV1 and FVC are stable, however the FEV25-75% has been falling for the last several months, which causes my doctors a little concern. *Most of the problems that come up with me at present are more related to side effects of medications or conditions I have acquired due to medications. *My swelling, aching feet and ankles and sore lower back are the main thing that effect me on a daily basis and sometimes keep me from doing things. Some of this is from medications and some from the chronic blood clot in my left leg that has never gone away. I really have to watch sodium intake also, as it increases the swelling. Sometimes the backaches limit me from the amount and type of exercise I can and want to do. Staying active, but not overdoing it is sometimes a thin line. *Although my lungs are doing well, as I mentioned before, some of my spirometry numbers have fallen some recently. My doctors feel that most likely “whatever” got to my lungs originally may still me active in my body and responds to the steroids (Prednisone). They recently did a bronchoscopy to try to determine or rule out chronic rejection, which is sometimes the cause of falling numbers. My numbers are really to high to be having rejection but they are trying to determine the reason for the decrease. The bronchoscopy came back as “inconclusive”. At the present, they are just monitoring my numbers very closely, and they seen to be staying stable again the last couple of months. Therefore they are not presently trying to get me to any lower dose of Prednisone, and just recently raised my dose to see if it would keep my spirometry more stable. So far so good! I was taking 7.5mg of Prednisone daily and they have put me back up to 10mg daily. Prednisone is the culprit in causing my diabetes, my cataracts, and my lowered bone density, Osteopenia (just to name a few). *Cognition – Sometimes I notice that I have very poor memory, especially short-term memory and ability to concentrate. Sometimes my thought process just doesn’t seem to work right! This may be medication related or possibly due to my blood sugar levels being unstable (highs and lows). I have noticed that many transplant patients I have contact with notice this same type of problem and there are many different theories as to the reason for this among us and among doctors. * I keep good records and a daily journal of doctors appointments, medical related phone calls, what I did for the day, and how I have felt that day. This comes in handy if you have something come up and the doctor says, how long have you had this headache, or when did you notice your leg was swelling more, etc. Sometimes when you read back it helps you to realize why something may be happening, such as you started a new medication and three days later you notice you are not feeling up to par. There is so much to remember, it always helps me to write things down.
My Next Big Adventure
I am always trying to challenge myself, and set new goals and find new adventures. A while back some of my friends in various support groups (both internet support and at my hospital) started talking about the U.S. Transplant Games. This is an event held in the US every two years to celebrate organ donation and organ transplantation. Transplant recipients participate in Olympic style games through friendly competition. It is a BIG event in the “transplant world”. I have known others who have participated and told me how exciting it is to be a part of “the games”. Not just transplant recipients attend, but also many donor families, some attending with the transplantee that received their loved ones gift of life. So this event is not just physical, but very, very emotional! I had thought about attending but never really seriously. Then Dr. Garnett said to me, while talking about some of my activities, ” You should go to the games!”. I tossed it around, and mulled over it and talked to my husband and my family and many others and as it looks now….. I AM GOING! I am pre-registered and I am signed up for individual bowling and team bowling. I am very excited about going! I have never traveled much, never flown in a commercial airline ( just a little two seater, open cockpit, stunt plane that did dips, and twists, and barrel rolls, but that’s a whole other story!) The games this year are in Minneapolis , Minnesota , July 27-August 1st. I am on Team Virginia (each state has a team). Besides participating, I will also be able to meet many of the people I talk to and have met online, who are also attending! It should be very exciting!
My Reason For Writing My Story
If you have made it this far, I commend you for sticking with me, as my story has turned out MUCH longer than I intended! If you are reading this, you may be waiting for a transplant or you have had one or you may be reading this for some other reason. Whatever the reason you read my story I just want you to know that I wrote it not to discourage anyone with all the things that can go wrong with transplants or chronic illnesses, but on the contrary, to encourage you, by seeing what we all can over come! Having this transplant is so worth it, I would do it again despite the hard times. If you are going through some tough times, struggles, things you hadn’t anticipated, or feel like it would be easier to just give up, please……. DON’T GIVE UP! You may be going through the “bumps” in the road or maybe they are “boulders”, as I often thought. You may feel like one step forward results in 3 or 4 backwards and this is very disheartening to say the least. It is easy to fall into depression, which can lead to inactivity, more sickness, and not following your doctors orders or medications, which can be your demise. ~ Hang in there. ~ Keep pushing yourself. ~ Set goals. ~ Don’t just settle for where ever you are now no matter what level of health you have. ~ Discipline yourself. ~ Make yourself, FORCE yourself to have a positive attitude. ~ When you feel overwhelmed just put one foot in front of the other and one day at a time and don’t give up! As in my case, a bad start and difficulties after transplant does not necessarily mean bad outcomes down the road! It may be weeks, months or more, but things can turn around. In my case, my first year was medically awful (my viewpoint), the next year was a lot better (but still not great). Now over three and a half years post transplant my life is so much better than I had ever anticipated it could be! (Ok, knock on wood!) It took me a while to realize, “Hey, you are not so sick anymore, get up off your butt and see what you are capable of doing!” I want to reap the rewards of these great new lungs! Who knows what awaits me in the future. I know God has something He wants me to do and I hope I can accomplish it. I am realistic and know that things could change tomorrow, BUT I am living for today!—-Irene Bailey Overton
“Life may not be the party we had hoped for, but while we are here, we might as well dance!
If you have any questions or comments please feel free to contact me at iboverton@simflex.com. I would love to hear from you!


